2.3.1 Parasternal window - Long-axis views (PLAX)
For the parasternal window, you have to position the patient on his/her left side and place the transducer in the 3rd or 4th intercostal space on the left side right next to the sternum.

2.3.1.1 Standard parasternal long-axis view
For the parasternal long-axis view, the marker of the transducer points somewhat towards the right shoulder. The exact orientation depends on the axis of the patient’s heart. If the patient is slim and the heart axis is steep, rotate the transducer a little further in a clockwise direction - in obese and pyknic patients, the transducer must be rotated a little in a counterclockwise direction.
Usually, you will not be able to see the apex in this view, and you should try to display the left ventricle as long stretched as possible (meaning a maximum cranial to caudal length on your screen), the depth being adjusted so that the left ventricle fills your screen with about one centimeter at the bottom for the structures posterior of the left ventricle. In an optimal PLAX view, there is just a small or no angle between the anterior wall of the aorta and the septum. An angle between these structures is usually the result of an excessively low imaging position.
As you will see later, an angle denotes that the ventricle is imaged in an oblique orientation, which would lead to false M-Mode measurements. Although the PLAX views cannot be used for M-Mode measurements, you can still interpret the 2D findings using eyeballing.
The PLAX view provides a lot of substantial information: Although the apical segments of the heart are not visible, you will get a good overview of cardiac function. Specifically, it allows you to interpret the morphology and motion of the interventricular septum, and you can also see the aortic root and the left atrium in this view - the size of the aorta should be measured right here. To inspect the more cranial portions of the aorta, you will have to move the transducer up one intercostal space. Since only a small portion of the right ventricle can be seen, PLAX is not an ideal view to interpret RV function.
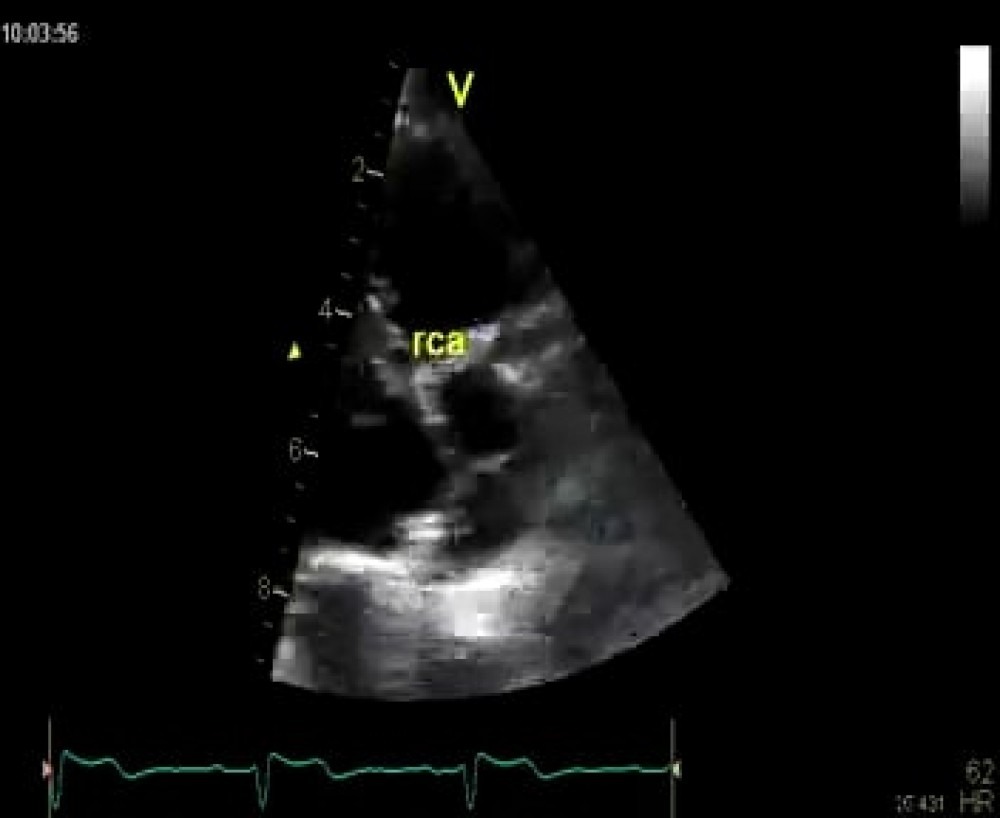
If the image quality is good you will also be able to see the right coronary artery at its origin in the right coronary sinus:
The PLAX view also permits measurement of the size of the left atrium (especially in its anterior/posterior extension) and is also very important for the interpretation of valvular function. Since we are very close to the aortic and the mitral valve, you can view details of both valves and the subvalvular apparatus of the mitral valve (papillary muscle, chordae) - just tilt the transducer back and forth, parallel to the long-axis, to view these structures.
Additional structures that can be seen in the PLAX view are the coronary sinus (at the junction between the left atrium and the left ventricle) and the descending aorta (behind the left atrium).
By increasing the depth on your ultrasound machine, you can even have a look beyond the posterior wall of the heart from this position, assessing for pleural or pericardial effusion.
2.3.1.2 Parasternal long-axis of the RV (PLAX-RV)
For this view, coming from the standard PLAX view, you simply have to tilt the transducer more towards the right of the patient. This view is probably the best to display the tricuspid valve. In addition to the good image quality of the valve, we will be able to name the individual leaflets: the anterior leaflet is seen in the near field, the posterior leaflet in the far field of the imaging sector, so use the PLAX -RV view to assess the tricuspid valve!
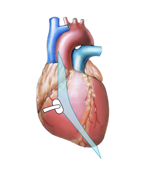
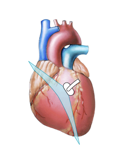
| PLAX - LV | PLAX - RV |
|---|---|
 |  |
 |  |
Comparison: Standard parasternal long-axis (left) and parasternal long-axis of the right ventricle
Coming from the PLAX view of the left ventricle, you can also tilt the transducer anteriorly and rotate slightly clockwise to visualize the right ventricular outflow tract and the pulmonary valve with the proximal part of the pulmonary artery. In some cases, you might even be able to image the bifurcation of the pulmonary artery.